ROCHESTER, N.Y. — Nearly one million Americans are suffering from Parkinson’s disease. The brain disorder can cause uncontrollable movements and shaking, and as the disease progresses over time, it can make walking and talking difficult. Around 90,000 Americans are diagnosed with Parkinson’s each year, and more than 1.2 million are expected to have the disease by 2030. With more people being diagnosed with the debilitating disease, the question medical professionals ask is, what is triggering the disorder? Researchers from the University of Rochester believe common environmental toxicants — inhaled or ingested — could be setting off the disease in different ways, leading to distinct subtypes of Parkinson’s.
The hypothesis, published in the Journal of Parkinson’s Disease, builds on the “brain-first vs body-first” model of Parkinson’s disease. This model suggests that the disease can start in two places: the brain, beginning in the olfactory bulb (involved in smell), or the body, originating in the nervous system of the gut.
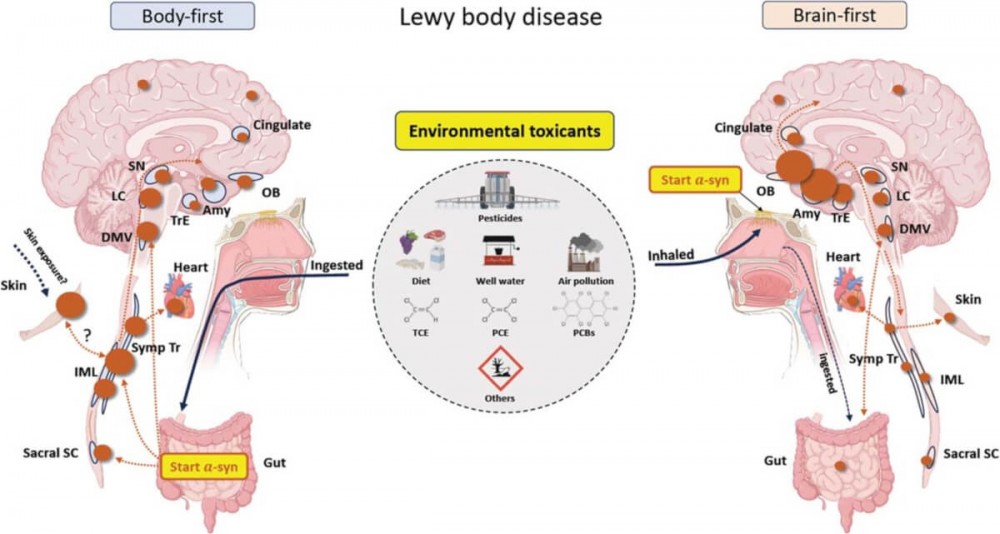
“In both the brain-first and body-first scenarios the pathology arises in structures in the body closely connected to the outside world,” says study co-author Dr. Ray Dorsey, a professor of neurology at the University of Rochester Medical Center, in a media release. “Here we propose that Parkinson’s is a systemic disease and that its initial roots likely begin in the nose and in the gut and are tied to environmental factors increasingly recognized as major contributors, if not causes, of the disease. This further reinforces the idea that Parkinson’s, the world’s fastest growing brain disease, may be fueled by toxicants and is therefore largely preventable.”
From these starting points, the disease process, marked by clumps of a protein called alpha-synuclein, spreads in a predictable way. Brain-first cases have early movement problems and only later develop issues like constipation. Body-first cases tend to have early features like sleep disorders and a more symmetric onset of motor symptoms.
So, what might cause alpha-synuclein to misfold and aggregate in the first place? University of Rochester researchers propose that in brain-first Parkinson’s, inhaled toxicants could be the culprit. Pesticides like paraquat, used in farming, are strongly linked to the disease and seem to enter the brain through the nose. Similarly, toxic solvents like trichloroethylene (TCE) and perchloroethylene (PCE), used in dry cleaning, can off-gas into the air and be inhaled. Even air pollution itself, especially tiny particulate matter, has been tied to Parkinson’s risk.
In contrast, researchers propose that in body-first disease, ingested toxicants could be triggering alpha-synuclein clumping in the gut. Pesticides can contaminate well water and the food supply. Drinking well water is linked to Parkinson’s, and specific pesticides are tied to body-first features like REM sleep behavior disorder. Industrial chemicals like TCE can also pollute groundwater. Notably, a recent study found a 70 percent higher Parkinson’s risk in Marines at Camp Lejeune, where drinking water was contaminated with TCE for over 30 years.
“These environmental toxicants are widespread and not everyone has Parkinson’s disease,” explains Dr. Dorsey. “The timing, dose, and duration of exposure and interactions with genetic and other environmental factors are probably key to determining who ultimately develops Parkinson’s. In most instances, these exposures likely occurred years or decades before symptoms develop.”
The idea generates testable predictions. Researchers hypothesize that Parkinson’s prevalence will track with toxicant exposure in different regions — inhaled toxicants correlating with brain-first disease and ingested with body-first. Therefore, as some countries curb the use of concerning chemicals, cases may fall, while in industrializing nations with worsening pollution, rates may rise. Affected individuals should show distinct brain imaging patterns based on the toxicant route. In animal studies, inhaled toxicants should trigger a brain-first distribution of alpha-synuclein pathology, while ingested should provoke a body-first pattern.
What can be done to combat this? Researchers have a handful of ideas, including:
The clues to preventing Parkinson’s may be right under — or up — our nose. As neuroscientists work to unravel this brain disorder, the search may lead us to take a closer look at the air we breathe and the environment we live in.
Parkinson’s Disease Treatments: Understanding Your Options
While there is currently no cure for Parkinson’s, there are several treatment options available to manage symptoms and improve quality of life.
Medications
Surgical Treatments
Lifestyle Modifications
Complementary Therapies
Experimental Treatments
Treatment plans for Parkinson’s disease are tailored to each individual’s specific needs and may involve a combination of therapies. Working closely with a healthcare provider who specializes in movement disorders is essential for developing an effective treatment strategy. As research continues, new therapies may emerge, offering hope for better symptom management and, ultimately, a cure for Parkinson’s disease.







